刀剑江湖路
《刀剑江湖路》是一款武侠RPG,传统武侠剧情混合沙盒内容,体验横版即时战斗。玩家扮演一名寻常少年,陷入江湖武林的血雨腥风,在纷争中成就侠名,搅动天下大势,成为万人敬仰的大侠。》》》订阅创意工坊热门MOD体验倍增!
现在下载
《刀剑江湖路》是一款武侠RPG,传统武侠剧情混合沙盒内容,体验横版即时战斗。玩家扮演一名寻常少年,陷入江湖武林的血雨腥风,在纷争中成就侠名,搅动天下大势,成为万人敬仰的大侠。》》》订阅创意工坊热门MOD体验倍增!
现在下载
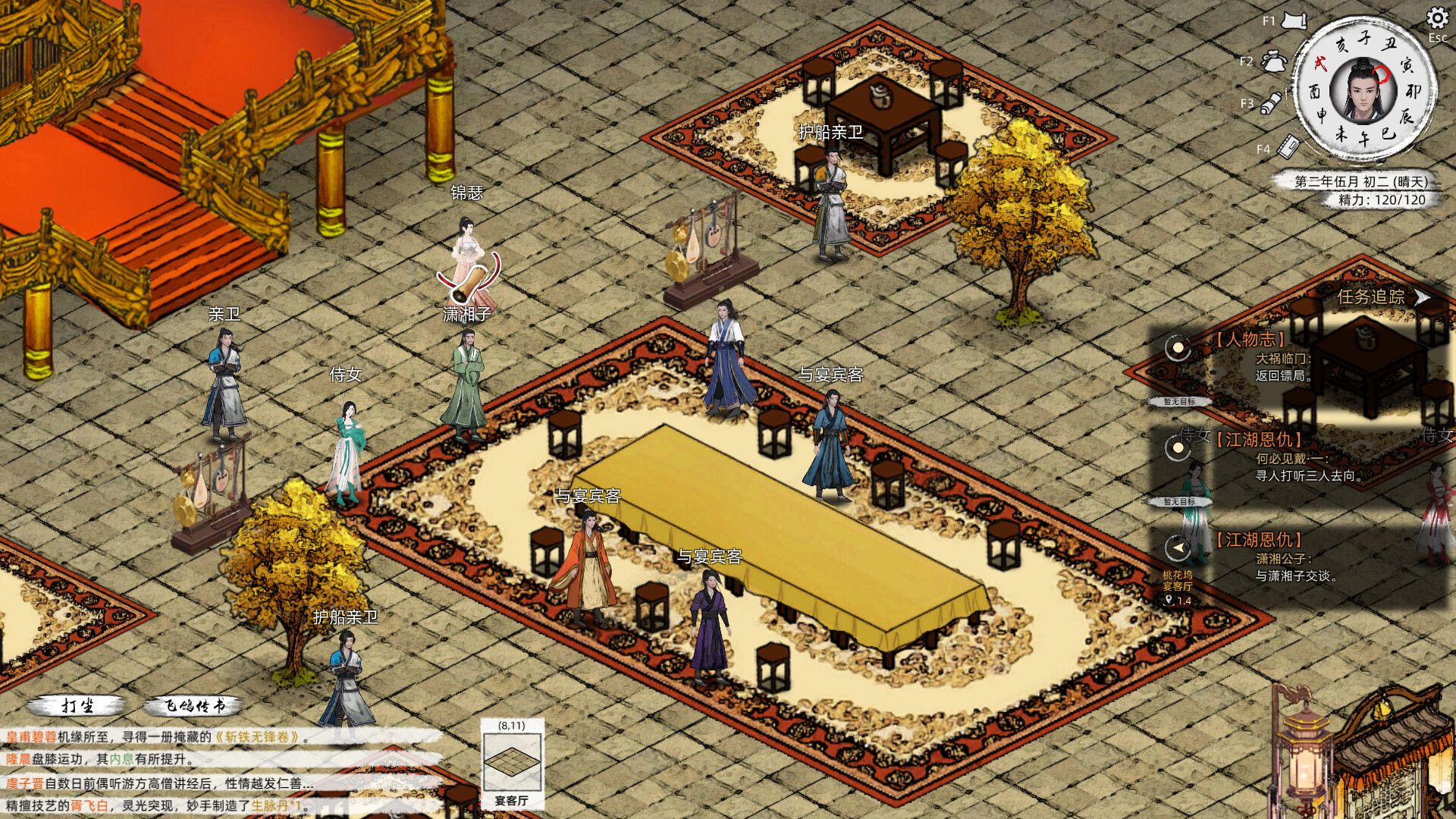
【4月29日EA转正,正式上线】
EA至今7个多月,在经过了近30次更新,推出了3个重大版本更新后,《刀剑江湖路》正式转正,完结主线剧情(五大结局)&推出沙盒内容,后续推出【免费DLC】
註:Steamdeck需要在正式版上线后再逐步做适配,目前体验一般

【正式版】内容包括:
主线&支线:15个大地图(5个门派)以及其他小地图,百万+剧情文案
武学:十余种兵器,数十套武学/轻功/内功、武学混用、神功、三才书系统、天赋等
帮派玩法:自建帮派、帮派战争、吞并帮派、收服帮派等
NPC互动:同伴、仇家、家仆、生育等
其他重要玩法:武林大会、随机事件、生活、钓鱼、青楼、赌坊、地牢、捕快、杀手等
【后续更新计划】
后续重点更新:逐步增添&完善沙盒内容以及机制、更新创意工坊2.0、更新免费DLC等
从江湖中的无名之辈伊始,以微末之身,于诡谲的江湖纷争中成就侠名,搅动天下大势。
——百万字的原创武侠剧情,主线五大结局,沈浸式体验江湖恩怨情仇

——15个地图,包含5个大门派剧情,解锁不同的江湖故事
——结交不同性格的江湖人物,与不同的江湖人士互动,或红尘相伴,或传授武艺,或图谋不轨、心狠手辣
系统需求
最低配备:
作业系统: Windows 10 64 bit
处理器: 2.5GHz
记忆体: 8 GB 记忆体
显示卡: HD4400
DirectX: 版本:11
储存空间: 20 GB 可用空间
建议配备:
作业系统: Windows 10 64 bit
处理器: Intel i5

记忆体: 16 GB 记忆体
显示卡: NVIDIA 1050
DirectX: 版本:11
储存空间: 20 GB 可用空间


